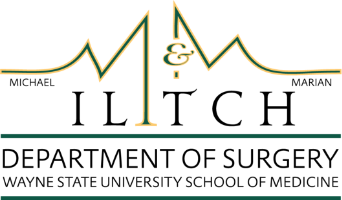History of Surgery at WSU
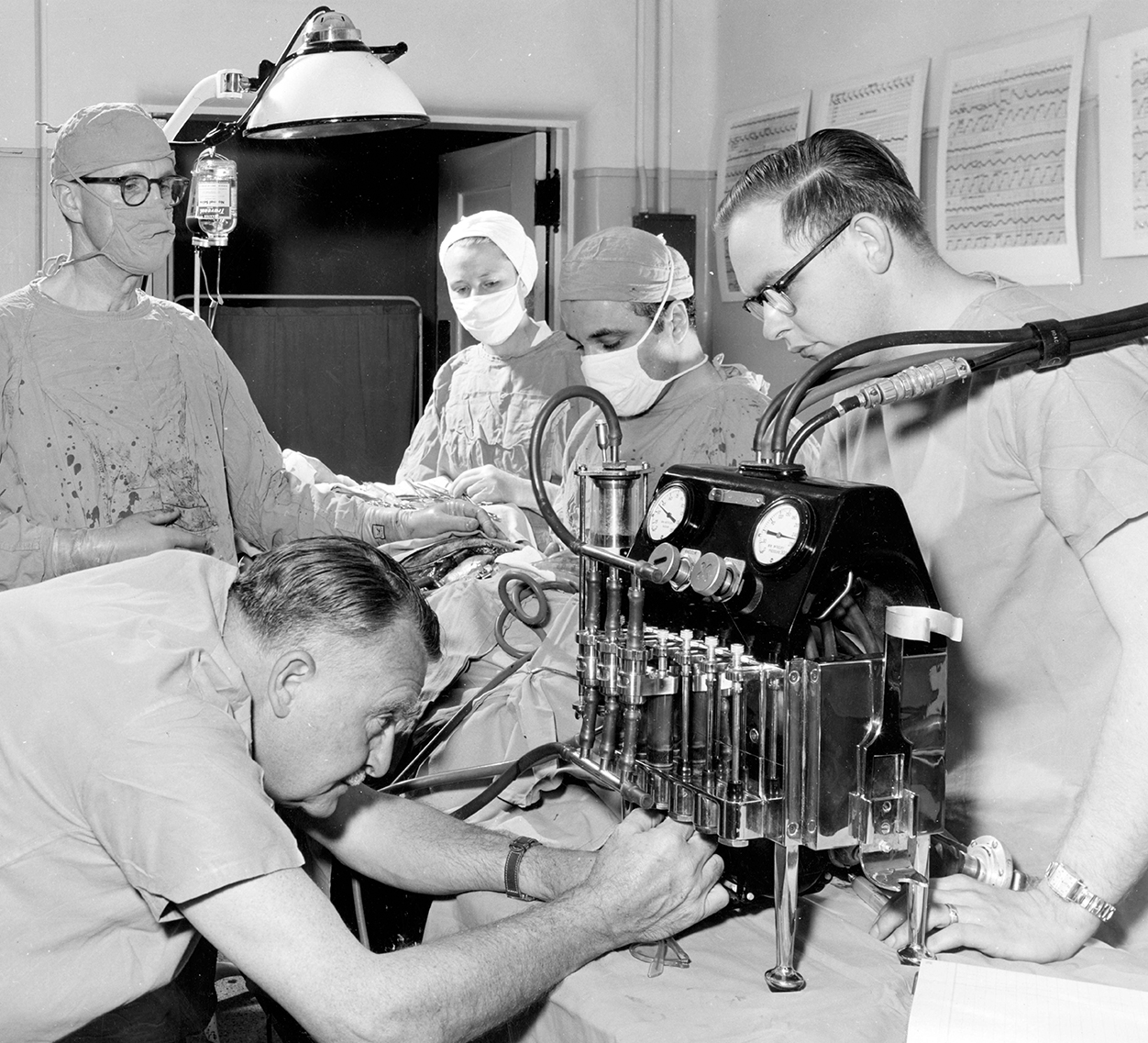
The Ilitch Department of Surgery at Wayne State University School of Medicine has a rich and proud tradition of leadership in the field of surgery, from the first successful open heart surgery in the world to Detroit’s first African American general surgeon. Here are some highlights.